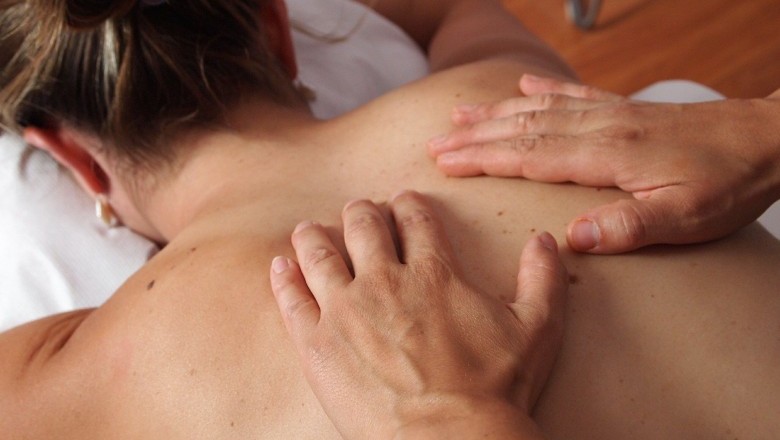
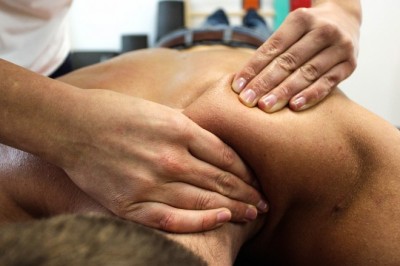
Helping Shoulder Fractures by using Physiotherapy
Fractures of the humerus are common and make up about 5% of all fractures, with 80% of them either undisplaced or just minimally displaced. More common in people suffering from osteoporosis, it is common to have a forearm fracture on the same side. Damage to the nerves or circulatory system is possible from these fractures but not often seen. Common areas of fracture are the neck of humerus at the top of the arm(fractured shoulder) and the mid shaft of the arm bone.
A fall onto the outstretched hand, onto the elbow or onto the shoulder itself is the most common cause of a fractured arm. Since many of the arm muscles insert onto the humeral head, when the injury occurs the muscular action involved can displace the fragments and complicate the management. 65 years old is the peak incidence for this kind of fractured humerus and if younger patients suffer this fracture the likely cause will involve high forces such as traffic accidents or sports injury.
If the fracture occurred without significant force then a pathological cause such as cancer must be suspected. On physio examination pain will occur on movement of the shoulder or the elbow, there may be extensive bruising and swelling, the arm may appear short if the fracture is displaced in shaft fractures and there is very restricted shoulder movement. Radial nerve damage is rare in upper humeral fractures but more common in fractures of the shaft, leading to "wrist drop", weakness of the wrist and finger extensors and some thumb movements.
Shoulder Fracture Management
Initial management is to restrict the patients movement and give them enough painkillers to make them comfortable. Upper humeral fractures can be managed conservatively if not displaced but if the greater tuberosity is fractured then an injury to the rotator cuff must be considered, more common in older people, injuries with high forces involved and where there is a lot of displacement. The typical treatment is a collar and cuff sling, allowing the elbow to hang in mid air and keep the humerus in line. Shaft fractures may be managed by humeral bracing.
Fractures with three or four parts plus displacement often need surgical treatment, with open reduction surgical fixation (ORIF) more often required in younger patients. In older people the humeral head may be replaced as the fracture may not heal or give an acceptable pain or movement result. Shaft fractures usually heal without surgery (plating or nailing) and are managed in a functional brace. Complications include frozen shoulder, avascular necrosis of the humeral head in multi-part fractures and nerve injury in shaft fractures. Six to eight weeks is typical healing time with older people often suffering a permanent reduction in shoulder movement.
Physiotherapy Management of Shoulder Fractures
Initially the physio assesses the arm, asking the patient about their pain level as this varies greatly, examining the swelling and bruising of the arm. The physiotherapist then checks the available range of movement of the shoulder, elbow, forearm and hand. Any muscle weakness and sensory loss is noted as this may denote nerve damage. If not operated on, a sling is continued with and if the fracture is not too painful or severe, early exercises are started by the physiotherapist. Pendular exercises, with the patient bending over at the waist, are important in the early stages as they allow movement of the shoulder joint without much force.
Once the three week stage is reached the fracture will have begun to heal and auto-assisted exercises can be started, where the patient helps the affected arm with the uninjured one. This is progressed to unassisted exercises, moving the arm up above the head, behind the back and behind the neck. As the six week point approaches, when the bone has effectively healed, the physiotherapist will start the patient doing more forceful exercises involving gentle stretches at the end of range to improve mobility. Mobilisation techniques to the shoulder joint and strengthening exercises using Theraband are progressed to increase muscle power and joint range.
Jonathan Blood Smyth is a Superintendent
Physiotherapistat an NHS hospital in the South-West of the UK. He specialises in orthopaedic conditions and looking after joint replacements as well as managing chronic pain. Visit the website he edits if you are looking for
physiotherapists in London.