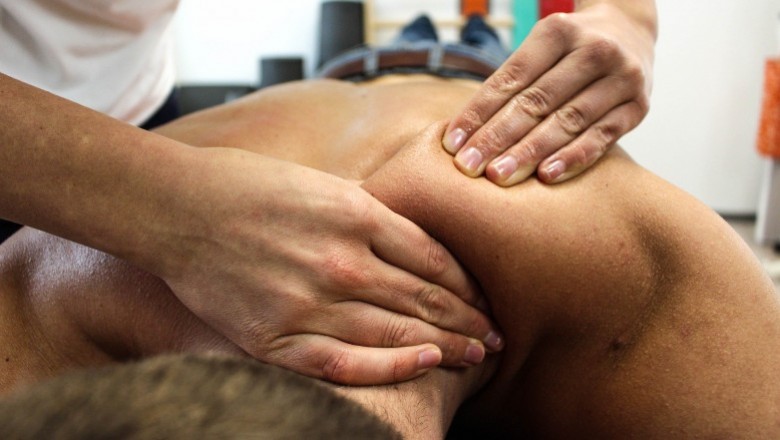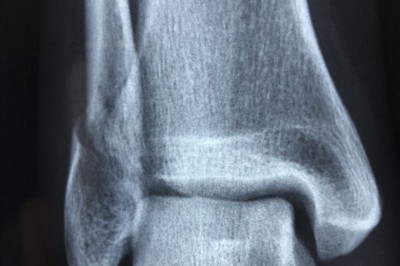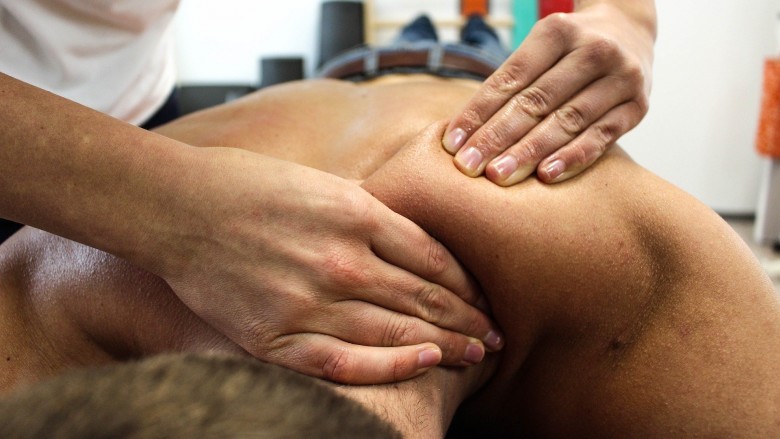
The Treatment of Wrist Fractures by Physiotherapists
How Physiotherapists Treat Wrist Fractures
by Jonathan Blood Smyth
Every winter the weather gets cold and icy at some time and we realise that the time has come when we are less safe out and about, that season when people start to slip and fall. Falls on an outstretched hand (FOOSH) are a very common injury and often cause a fracture of the end of the forearm bones, a fracture routinely known as a wrist or colles fracture. The fracture can be insignificant or very major requiring screws and plates to realign and fix it in position. Physiotherapists assess and plan rehabilitation of the wrist, hand and forearm.
The wrist is the most commonly damaged part of the arm and three quarters of wrist injuries consists of radius and ulna fractures. Minor injuries may have just a crack and remain in position and as injuries become more serious they involve larger numbers of fragments and more marked displacement. As the person falls on the hand the results depend to some degree on age: children develop a greenstick fracture (a kink in the bone), adolescents separate the growth plate from the bone and adults fracture the radius and ulna in the last inch near the wrist.
The commonest age groups for colles fractures to occur in are the 6-10 and the 60-69 year olds, with older people more likely to suffer fractures in the forearm away from the joint and younger people, due to the higher violence of the injury, being more likely to get joint involvement in the fracture. Diagnostic features of a radius and ulna fracture are significant pain with increased pain on palpating the area, a "dinner fork" bony deformity, swelling over the area and a marked reluctance to use it.
Orthopaedic Management of Wrist Fracture
To allow the fracture to heal correctly a colles fracture needs to be fixed in a position that allows the fracture to be held in as close to the original shape as possible. A simple fracture which is undisplaced can just be plastered and left to heal, while a displaced fracture has to be returned to a better anatomical alignment. Manipulation and plastering might work, but if the fracture does not remain in a good position then operative fixation with k-wires or plates and screws might be required. After the operation plaster is applied to maintain the correction.
Physiotherapy Rehabilitation of Wrist Fractures
The plaster is usually in place for 5-6 weeks and then the physiotherapist can get a look at the wrist and hand to see what rehabilitation plan is required. When the hand is removed from plaster its condition varies greatly so a skilled physio needs to assess the situation and recommend appropriate treatment. The swelling and colour of the hand will give the physiotherapist important information about how severe things are. High levels of pain, strong changes in colour and extreme swelling in the hand and wrist could indicate Complex Regional Pain Syndrome (CRPS), a severe pain condition needing vigorous management.
The physio will look at the ranges of movement of the upper limb, checking the shoulder ranges first to make sure the shoulder was not damaged in the fall. The elbow range is usually unaffected except in some cases where the patient has kept their elbow bent in a sling for weeks, making the joint stiff. Supination and pronation are very important movements functionally and often restricted due to the proximity of the inferior radio-ulnar joint to the fracture site. Wrist flexion and extension, finger movement and thumb ranges are all assessed and recorded.
If the assessment shows only a stiff and uncomfortable wrist the physiotherapy exercises will consist of range of movement for the shoulder, elbow, forearm rotation, wrist and hand. To ease the transition out of plaster and enable early functional ability without pain a velcro futura wrist splint can be used for a week or so. Referral to exercise hand class may be necessary and the physios can mobilize the wrist and forearm joints by re-establishing the gliding movements between the joints. As the wrist improves the focus of physio moves to strengthening exercises and the promotion of normal day-to-day activities.
Jonathan Blood Smyth is a Superintendent
Physiotherapistat an NHS hospital in the South-West of the UK. He specialises in orthopaedic conditions and looking after joint replacements as well as managing chronic pain. Visit the website he edits if you are looking for
physiotherapists in Glasgow.